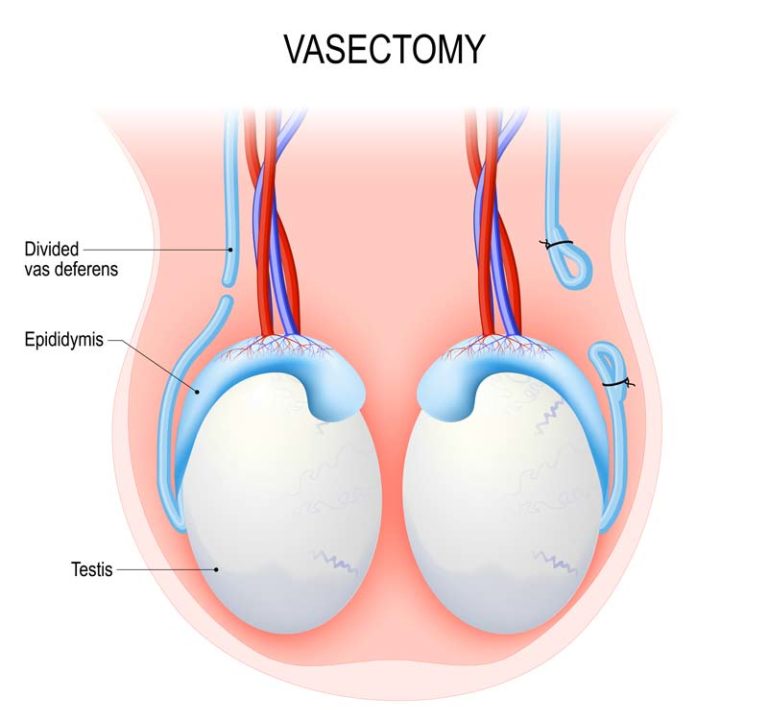
What is a Vasectomy?
A vasectomy is a minor surgical procedure that prevents the release of sperm in semen. Semen is still produced, but it no longer contains sperm. The testes do continue to produce sperm, but they are absorbed by the body. A vasectomy is a popular form of birth control, with over 500,000 men choosing it each year.
It is one of the most effective forms of birth control, with a success rate of about 99.8%. It’s also permanent unless a man decides to have a vasectomy reversal procedure.
How Does a Vasectomy Work?
The testes, or testicles, produce both sperm and male sex hormones like testosterone. When sperm are manufactured, they are stored in a coiled tube called the epididymis, which is connected to the prostate by the vas deferens, or vas. The vas deferens is responsible for moving sperm out of the testes so it can be mixed with the seminal fluid made by the seminal vesicles. During ejaculation, semen is formed by the mixture of seminal fluid and sperm, and it travels through the urethra and exits the penis.
Since the vas deferens is the tube that carries sperm out of the testicles, cutting it and sealing the two ends ensures that sperm can no longer exit.
Procedure
Vasectomies are often performed in a urologist’s office. They may also be done at a surgery center or hospital. The choice of location may depend on factors such as the patient’s preference, level of anxiety, and the need for sedation. In some cases, patients may opt for sedation to make the procedure more comfortable, and this may require the procedure to take place in a surgery center or hospital.
However, some urologists offer inhaled nitrous oxide, which can be administered in the office without the need for full anesthesia or injectable sedation.
Before the procedure, patients may be required to sign a consent form, which varies depending on state laws.
During the procedure, the scrotal area will be cleaned and numbed with a local anesthetic to minimize pain. However, patients may still feel pressure, touch, and movement. Some men choose to use inhaled nitrous oxide, or laughing gas, to provide additional relaxation and relief.
Vasectomy Types
Conventional Vasectomy
A conventional vasectomy involves making one or two small incisions in the scrotum to access the vas deferens. The vas deferens is then cut and a small section may be removed, creating a small gap between the two ends. The urologist may then cauterize the ends of the vas and tie the cut ends with a suture. This process is repeated on the other vas deferens through the same or a separate incision. The incisions in the scrotum may be closed with dissolvable stitches or left to heal on their own.
No-Scalpel Vasectomy
During a no-scalpel vasectomy, the urologist uses a small clamp to locate and hold the vas deferens through the skin of the scrotum. Instead of making a large incision, a small hole is made in the skin and widened to access the vas deferens. The vas is then cut, tied, or cauterized and returned to its original position.
Vasectomy Risks
Immediately after the surgery, there is a slight chance of bleeding in the scrotum. If you experience an increase in scrotal size or pain, contact your urologist immediately. If there is a fever, redness, or soreness in the scrotum, it may indicate an infection and you should seek medical attention.
Post-vasectomy pain syndrome (PVPS) is a rare complication characterized by persistent pain following the procedure. The cause of PVPS is unknown, but it is often treated with anti-inflammatory medications. Some men may choose to reverse the procedure to alleviate the pain, but this does not always provide a solution.
Research has shown that there is not increased risk of heart disease, prostate cancer, testicular cancer, or other health issues in men who have undergone a vasectomy.
Vasectomy Recovery and Follow Up
After the procedure, you should rest at home. You should also avoid strenuous activities and sexual intercourse until you have fully recovered. Ice packs and a supportive undergarment such as a jockstrap can help to reduce swelling and pain. Most men fully recover within a week and are able to return to work the next day.
You may experience some discomfort, which is usually managed with over-the-counter pain medication. However, severe pain may indicate an infection or other complications, and you should seek medical attention. A benign lump (granuloma) may form due to leaked sperm from the cut vas deferens, which may be painful or sensitive to touch, but it is not harmful and typically improves over time.
It’s important to note that a vasectomy does not work immediately and sperm may still be present in the semen for around 3 months or 20 ejaculates. Your urologist will give you instructions on how to follow up with semen analysis to confirm the absence of sperm in your ejaculate.
It is essential to use alternative forms of birth control until your semen analysis confirms there is no longer sperm. In some cases, it may take longer for the sperm to clear and a vasectomy should not be considered effective until a semen analysis confirms that it is.
Frequently Asked Questions
Is it noticeable if I have had a vasectomy?
Sperm makes up a small portion of semen, so there should be no noticeable change in the volume of your ejaculate after a vasectomy. In rare cases, your partner may be able to feel the procedure site, particularly if a granuloma has formed.
Will a vasectomy affect how an orgasm feels?
Vasectomy typically does not affect ejaculation or orgasm. However, there are rare cases where men may experience pain during orgasm due to post-vasectomy pain syndrome.
Will a vasectomy cause impotence or erectile dysfunction?
A vasectomy, when performed without complications, does not cause impotence.
Can a vasectomy fail?
There is a slight possibility that a vasectomy may not be successful. This can occur if sperm leaks from one cut end of the vas deferens and finds a way to the other end.
Can a vasectomy be reversed?
Yes, a vasectomy can be reversed. The procedure is called vasectomy reversal and it involves reconnecting the vas deferens which were previously cut during the vasectomy procedure. However, it is important to note that the success of a reversal depends on many factors, including the length of time since the vasectomy, the method used for the original procedure, and the age and overall health of the patient. Additionally, the success rate of vasectomy reversal is lower than the initial vasectomy procedure, and there is no guarantee that it will restore fertility. In order to have the best chance of success, a urologist with specialized training and experience should be chosen.