What is Overactive Bladder (OAB)?
Overactive bladder (OAB) is the name for a group of urinary symptoms. It is not a disease. The most common symptom is a sudden, uncontrolled need or urge to urinate. Some people will leak urine when they feel this urge. Another symptom is the need to pass urine many times during the day and night. OAB is basically the feeling that you’ve “gotta’ go” to the bathroom urgently and too much.
Leaking urine is called “incontinence”. Stress urinary incontinence (SUI), is another common bladder problem. It’s different from OAB. People with SUI leak urine while sneezing, laughing or doing other physical activities. More information on SUI can be found on our SUI page.
Key Statistics
As many as 30 percent of men and 40 percent of women in the United States live with OAB symptoms. Many people living with OAB don’t ask for help. They may feel embarrassed. Many people either don’t know how to talk with their health care provider about their symptoms, or they think there aren’t treatments that can help.
The truth is there are many treatments that can help. Asking your health care provider about it is the first step.
How OAB Can Affect Your Life
OAB can get in the way of your work, social life, exercise and sleep. Without treatment, OAB symptoms can make it hard to get through the day without many trips to the bathroom. You may not want to go out with friends or go far from home because you’re afraid of being far from a bathroom. This makes many people feel lonely and isolated.
OAB may affect relationships with friends and family. It can disrupt your sleep and sex-life. Too little sleep will leave anyone tired and depressed. In addition, if you leak urine, you may develop skin problems or infections.
You don’t have to let OAB rule your life. OAB can be controlled. If you think you have OAB, see your health care provider.
The Truth About OAB
OAB is not a normal part of getting older.
OAB is not just part of being a woman.
OAB is not just an issue with the prostate.
OAB is not caused by something you did.
Surgery is not the only treatment for OAB.
There are treatments to help people manage OAB symptoms.
There are treatments to help even minor OAB symptoms.
If you are bothered by OAB symptoms, then you should ask for treatment!
Symptoms
Urgency: The major symptom of OAB is a sudden, strong urge to urinate that you can’t ignore. This “gotta go” feeling makes you fear you will leak if you don’t get to a bathroom right away. You may or may not actually leak with this urge to go.
If you live with OAB, you may also:
Leak urine or have “urge incontinence.” This means urine leaks when you feel the sudden urge to go. This isn’t the same as stress urinary incontinence or SUI . People with SUI leak urine when sneezing, laughing or doing other physical activities.
Urinate frequently. You may need to go to the bathroom many times during the day. The number of times someone urinates varies from person to person. Many experts agree that going to the bathroom more than eight times in 24 hours is “frequent urination.”
Wake up at night to pass urine. If you have to wake from sleep to go to the bathroom more than once a night, it’s a symptom of OAB or nocturia.
Causes
How the Urinary Tract Works Normally, and What Causes OAB
The urinary tract is the important system in our bodies that removes liquid waste (urine). It includes the organs that produce, store and pass urine. These are:
- Kidneys: two bean-shaped organs that clean waste from the blood and make urine.
- Ureters: two thin tubes that take urine from the kidney to the bladder.
- Bladder: a balloon-like muscular sac that holds urine until it’s time to go to the bathroom.
- Urethra: the tube that carries urine from the bladder out of the body. The urethra has a muscle called a sphincter that locks in urine.
- The sphincter muscle opens to release urine when the bladder contracts.
Normally, when your bladder is full of urine waste, your brain signals the bladder. The bladder muscles then squeeze. This forces the urine out through the urethra. The sphincter in the urethra opens and urine flows out. When your bladder is not full, the bladder is relaxed.
With a healthy bladder, signals in your brain let you know that your bladder is getting full or is full, but you can wait to go to the bathroom. With OAB, you can’t wait. You feel a sudden, urgent need to go. This can happen even if your bladder isn’t full.
If the nerve signals between your bladder and brain don’t work properly, OAB can result. The signals might tell your bladder to empty, even when it isn’t full. OAB can also be caused when muscles in your bladder are too active. This means that the bladder muscles contract to pass urine before your bladder is full. In turn, this causes a sudden, strong need to urinate. We call this “urgency.”
Risk Factors for OAB
- Neurologic disorders or damage to the signals between your brain and bladder
- Hormone changes
- Pelvic muscle weakness or spasms
- A urinary tract infection
- Side effects from a medication
- Diseases that affect the brain or spinal cord, like stroke and multiple sclerosis
If you think you have OAB, talk with your health care provider. It’s important to learn why it’s happening so you can manage your symptoms.
Diagnosis
After you talk about your symptoms, your health care provider may do an exam right away. Or, they may refer you to a specialist, such as a urologist who can diagnose and treat OAB. Some urologists specialize in incontinence and OAB.
Medical History
Your exam will begin with questions. Your provider will want to understand your health history and experiences. You should tell them about the symptoms you have, how long you’ve had them, and how they’re changing your life. A medical history will include questions about your past and current health problems. You should bring a list of over-the-counter and prescription drugs you take. You should also tell your provider about your diet and about how much and what kinds of liquids you drink during the day and night.
Physical Exam
Your provider will examine you to look for something that may be causing your symptoms. Doctors will often feel your abdomen, the organs in your pelvis, and your rectum.
Bladder Diary
You may be asked to keep a Bladder Diary for a few weeks. With this, you will note how often you go to the bathroom and any time you leak urine. This will help your health care provider learn more about your day-to-day symptoms. The bladder diary helps you track:
- When and how much fluid you drink
- When and how much you urinate
- How often you have that “gotta go” urgency feeling
- When and how much urine you may leak
Having a Bladder Diary during your first visit can be helpful because it describes your daily habits, your urinary symptoms, and shows your provider how they affect your life. Your doctor will use this information to help treat you.
Other Tests
- Urine test: Your health care provider may ask you to leave a sample of your urine to test for infection or blood.
- Bladder scan: This type of ultrasound shows how much urine is still in the bladder after you go to the bathroom.
- More tests,like a cystoscopy or urodynamic testing, are usually not needed but may be used if your provider thinks something else is going on.
Treatment
There are a number of things you can do to manage OAB. Everyone has a different experience with what works best. You may try one treatment alone, or several at the same time.
You and your health care provider should talk about what you want from treatment and about each option. OAB treatments include:
- Lifestyle Changes
- Prescription Medications
- Bladder Botox® (botulinum toxin) Treatments
- Nerve Stimulation (peripheral and central)
- Surgery
Lifestyle Changes
For OAB treatment, health care providers may first ask a patient to make lifestyle changes. These changes may also be called behavioral therapy. This could mean you eat different foods, change drinking habits, and pre-plan bathroom visits to feel better. Many people find these changes help.
Other people need to do more, such as:
- Limit food and drinks that bother the bladder. There are certain foods and drinks known to irritate the bladder. You can start by avoiding diuretics – these drinks include caffeine and alcohol which encourage your body to make more urine. You can also try taking several foods out of your diet, and then add them back one at a time. This will show you which foods make your symptoms worse, so you can avoid them. You can add fiber to your diet to improve digestion. Oatmeal and whole grains are good. Fresh and dried fruit, vegetables, and beans may help. Many people feel better when they change the way they eat and drink.
Some foods and drinks that may affect your bladder:- Coffee/caffeine
- Tea
- Alcohol
- Soda and other fizzy drinks
- Some citrus fruits
- Tomato-based foods
- Chocolate (not white chocolate)
- Some spicy foods
- Keep a bladder diary. Writing down when you make trips to the bathroom for a few days can help you understand your body better. This diary may show you things that make symptoms worse. For example, are your symptoms worse after eating or drinking a certain kind of food? Are they worse when you don’t drink enough liquids?
- Double voiding. This is when you empty your bladder twice. This may be helpful for people who have trouble fully emptying their bladder. After you go to the bathroom, you wait a few seconds and then try again.
- Delayed voiding. This is when you practice waiting before you go to the bathroom, even when you have to go. At first, you wait just a few minutes. Gradually, you may be able to wait two to three hours at a time. Only try this if your health care provider tells you to. Some people feel worse or have urine leaks when they wait too long to go to the bathroom.
- Timed urination. This means you follow a daily bathroom schedule. Instead of going when you feel the urge, you go at set times during the day. You and your health care provider will create a reasonable schedule. You may try to go every two to four hours, whether you feel you have to or not. The goal is to prevent that urgent feeling and to regain control.
- Exercises to relax your bladder muscle.
- Kegel exercises: tightening and holding your pelvic muscles tight, to strengthen the pelvic floor.
- Quick flicks are when you quickly squeeze and relax your pelvic floor muscles over and over again. So, when you feel the urge to go, a number of quick flicks may help control that “gotta go” feeling. It helps to be still, relax and focus on just the exercise. Your health care provider or a physical therapist can help you learn these exercises.
- Biofeedback may also help you learn about your bladder. Biofeedback uses computer graphs and sounds to monitor muscle movement. It can help teach you how your pelvic muscles move and how strong they are.
Prescription Drugs
When lifestyle changes aren’t enough, the next step may be to take medicine. Your health care provider can tell you about special drugs for OAB.
There are several drug types that can relax the bladder muscle. These drugs, like anti-muscarinics and beta-3 agonists, can help stop your bladder from squeezing when it’s not full. Some are taken as pills, by mouth. Others are gels or a sticky transdermal patch to give you the drug through your skin.
Anti-muscarinics and betta-3 adrenoceptor agonists can relax the bladder muscle and increase the amount of urine your bladder can hold and empty. Combination drugs, like using both anti-muscarinics and – betta-3 adrenoceptor agonists together may help control OAB when one option alone isn’t working.
Your health care provider will want to know if the medicine works for you. They will check to see if you get relief or if the drug causes problems, known as side effects. Some people get dry mouth and dry eyes, constipation, or blurred vision. If one drug you try doesn’t work, your health care provider may ask you to take different amounts, give you a different one to try, or have you try two types together. Lifestyle changes and medicine at the same time help many people.
Bladder Botox Treatment
If lifestyle changes and medicine aren’t working, injections may be offered. A trained urologist for men and women, or a female pelvic medicine & reconstructive surgeon (FPMRS) can help with this. They may offer Bladder Botox Treatment.
Botox works for the bladder by relaxing the muscle of the bladder wall to reduce urinary urgency and urge incontinence. It can help the bladder muscles from squeezing too much. To put botulinum toxin into the bladder, your doctor will use a cystoscope passed into the bladder so the doctor can see inside the bladder. Then, the doctor will inject tiny amounts of botulinum toxin into the bladder muscle. This procedure is performed in the office with local anesthesia. The effects of Botox last up to six months. Repeat treatments will be necessary when OAB symptoms return.
Your health care provider will want to know if the botulinum toxin treatment works for you. They will check to see if you get relief, or if you aren’t holding in too much urine. If urine is not releasing well, you may need to use a catheter temporarily.
Nerve Stimulation
Another treatment for people who need extra help is nerve stimulation, also called neuromodulation therapy. This type of treatment sends electrical pulses to nerves that share the same path for the bladder. In OAB, the nerve signals between your bladder and brain do not communicate correctly. These electrical pulses help the brain and the nerves to the bladder communicate so the bladder can function properly and improve OAB symptoms.
There are two types:
Percutaneous tibial nerve stimulation (PTNS). PTNS (peripheral)is a way to correct the nerves in your bladder. PTNS is done by placing a small electrode in your lower leg near your ankle. It sends pulses to the tibial nerve. The tibial nerve runs along your knee to nerves in your lower back. The pulses help control the signals that aren’t working right. Often, patients receive 12 treatments, depending on how it’s working.
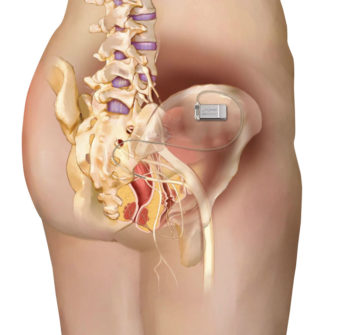
Sacral neuromodulation (SNS). SNS (central) changes how the sacral nerve works. This nerve carries signals between the spinal cord and the bladder. Its job is to help hold and release urine. In OAB, these nerve signals aren’t doing what they should. SNS uses a bladder pacemaker to control these signals to stop OAB symptoms. SNS is a two-step surgical process. The first step is to implant an electrical wire under the skin in your lower back. This wire is first connected to a handheld pacemaker to send pulses to the sacral nerve. You and your doctor will test whether or not this pacemaker can help you. If it helps, the second step is to implant a permanent pacemaker that can regulate the nerve rhythm.
Bladder Reconstruction/Urinary Diversion Surgery
Surgery is only used in very rare and serious cases. There are two types of surgery available. Augmentation cystoplasty enlarges the bladder. Urinary diversion re-routs the flow of urine. There are many risks to these surgeries, so it is offered only when no other option can help.
More Information
Providers and Specialists Who Treat OAB
Many types of health care providers can offer basic help for OAB. Here are the types of providers you may meet:
- Urologist* are surgeons who evaluate and treat problems of the urinary tract. Most urologists are very experienced with incontinence. However, not all of them specialize in treating OAB. A patient should ask if their provider specializes in treating OAB.
- Gynecologists are doctors who focus on women’s health. Most are knowledgeable about incontinence, but not all are trained to treat OAB.
- Female Pelvic Medicine and Reconstructive Surgery (FPMRS) specialists are urologists or gynecologists who are trained as experts in female pelvic health. The public often refers to FPMRS specialists as female urologists or urogynecologists.
- Primary Care Practitioners are doctors who can diagnose and treat common health concerns. If a primary care provider is experienced with OAB, they will tell you your options. Or, they may refer you to a specialist, especially if lifestyle changes haven’t helped.
- Internist are general doctors who may or may not be primary care providers. They will often refer to a specialist.
- Nurse Practitioners (NP) are highly trained nurses, able to treat many medical problems. Some NPs specialize in issues like OAB, or they will refer you to a specialist.
- Physician Assistants (PA) are professionals licensed to practice medicine with a doctor’s oversight. NPs and PAs are often part of the health care team. Many can diagnose and treat non-surgically and can help with exercises and lifestyle changes. Some specialize in issues such as OAB.
- Geriatricians are doctors who treat older patients, and many are able to evaluate and treat OAB. But, not all treat OAB.
- Physical Therapists are licensed health professionals who provide physical therapy. If they have special training in pelvic floor disorders, they can help with exercises and lifestyle changes for OAB.
*Typically, specialists who treat OAB and incontinence include urologists and female pelvic medicine specialists. It helps to ask if your health care provider has direct training or experience with OAB.
Tips for a Successful Doctor’s Visit
It’s normal to feel uncomfortable when talking about OAB symptoms. Who wants to talk about bathroom problems or incontinence? Still, knowing more about OAB is the best way to take control of the problem. A little planning will give you confidence. Here are some tips to help:
- Be prepared. Before your appointment, help the health care provider learn what’s going on by gathering some information. Also, be ready to take notes about what you learn. It is helpful to bring:
- A list of the prescription drugs, over-the-counter medicines, vitamins and herbs you take.
- A list of your past and current illnesses or injuries.
- A way to take notes about treatments.
- Bring a friend. Ask a close friend or relative to go with you to the doctor. An “appointment buddy” can help remind you of things you may forget to ask, or remind you of things the health care provider said.
- Bring up the topic. If your health care provider doesn’t ask about your OAB symptoms, then bring up the topic yourself. It may not be wise to wait until the end of your visit, so you can be sure you have time for questions. If a nurse meets with you first, tell the nurse about your symptoms.
- Speak freely. Share everything you’re experiencing. Your health care provider has heard it all! It’s okay to tell them about your symptoms and how they impact your daily life.
- Ask questions. A visit to your health care provider is the right time to ask questions. It is best to bring your list of questions with you so you don’t forget them. We offer some good questions to ask in each section of this guide to help you.
Talking with Your Health Care Provider
Questions to Ask the Doctor about OAB
- Are my symptoms from OAB or from something else?
- What tests will I need to find out if I have OAB?
- What could have caused my OAB?
- Can I do anything to prevent OAB symptoms?
Questions to Ask the Doctor about Treatment
- What would happen if I don’t treat my OAB?
- What lifestyle changes should I make?
- Are there any exercises I can do to help?
- Do I need to see a physical therapist?
- What treatment could help my OAB?
- How soon after treatment will I feel better?
- What are the good and bad things that I should know about these treatments?
- What problems should I call you about after I start treatment?
- What happens if the first treatment doesn’t help?
- Will I need treatment for the rest of my life?
- Can my OAB be managed?
- What are my next steps?
Questions to Ask Yourself about Symptoms
- Do my symptoms make me stop doing the things I enjoy, or prevent me from going to events?
- Am I afraid to be too far from a bathroom?
- Have my symptoms changed my relationships with friends or family?
- Do my symptoms make it hard to get a good night’s sleep?