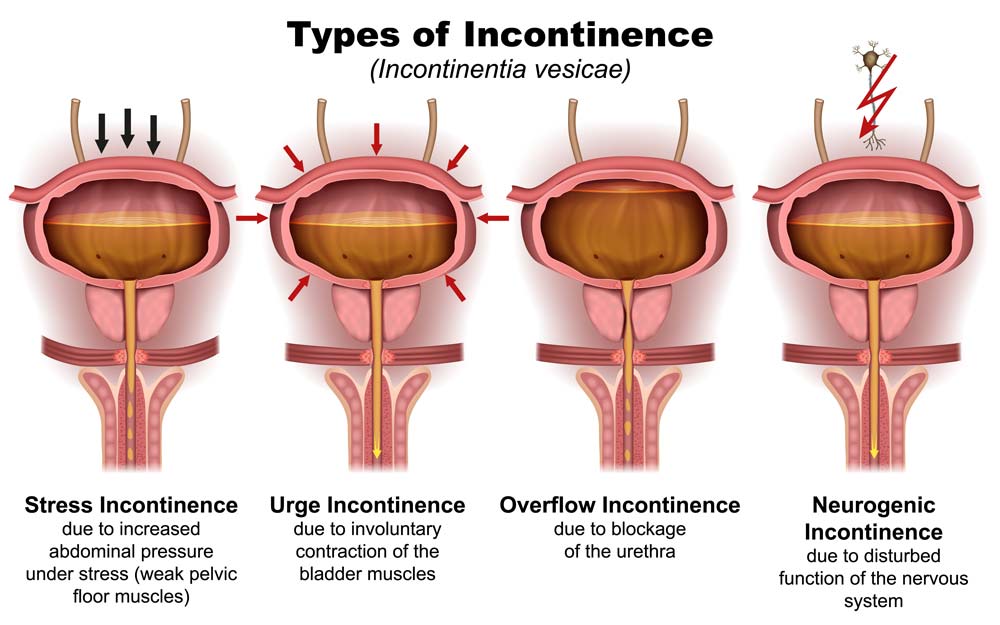
What Is Urgency Urinary Incontinence?
Urgency urinary incontinence (UUI) is a subtype of overactive bladder (OAB) syndrome. With UUI, you may experience a sudden, uncontrollable urge to urinate, resulting in urine leakage. This condition can occur during the day or night, often causing embarrassment, inconvenience, and limitations in your social and professional life.
Although UUI affects both men and women, treatment options are available to reduce your symptoms and restore your quality of life. Here’s everything you need to know about the basics of UUI.
Causes of Urgency Urinary Incontinence
The exact cause of urgency urinary incontinence is often unclear, but several factors can contribute to its development. These include:
- Neurological disorders: Conditions like multiple sclerosis, Parkinson’s disease, and stroke can affect the nerves controlling bladder function, leading to UUI.
- Bladder abnormalities: Bladder stones, tumors, or inflammation can irritate the bladder, causing increased urgency and involuntary urine loss.
- Hormonal changes: Reduced estrogen levels in postmenopausal women can weaken the pelvic floor muscles, resulting in UUI.
- Medications: Some medications, such as diuretics, antihypertensives, and antidepressants, can cause or worsen UUI.
- Infections: Urinary tract infections can irritate the bladder, leading to increased urgency and incontinence.
- Obesity: Excess weight can put pressure on the bladder and pelvic floor muscles, contributing to UUI.
- Aging: As we age, our bladder’s capacity to hold urine decreases, and the muscles that control urination weaken, increasing the risk of UUI.
Diagnosis of Urgency Urinary Incontinence
To diagnose urgency urinary incontinence, your provider will take a detailed medical history, perform a physical examination, and may order additional tests. Some common diagnostic tests include:
- Bladder diary: Patients are asked to maintain a record of their fluid intake, frequency of urination, and incontinence episodes.
- Urinalysis: A urine sample is analyzed for signs of infection, blood, or other abnormalities.
- Post-void residual (PVR) measurement: This test measures the amount of urine left in the bladder after urination, which can help determine if incomplete bladder emptying contributes to UUI.
- Urodynamic testing: A series of tests that assess the bladder’s function and capacity and the pressure and flow of urine during urination.
- Cystoscopy: A thin, flexible tube with a camera is inserted into the urethra to visualize the bladder’s interior and identify abnormalities.
- Imaging: Ultrasound, X-rays, or magnetic resonance imaging (MRI) may be used to evaluate the bladder, kidneys, and surrounding structures.
Treatment Options for Urgency Urinary Incontinence
There are a variety of treatment options available for managing urgency urinary incontinence, ranging from conservative approaches to surgical interventions. Your treatment choice depends on the severity of the condition, the underlying cause, and your preferences. Common treatment options include:
- Lifestyle modifications: Certain lifestyle changes, such as reducing caffeine and alcohol intake, maintaining a healthy weight, and adopting a regular urination schedule, can help improve the symptoms of UUI.
- Pelvic floor muscle exercises: Also known as Kegel exercises, these exercises help strengthen the muscles that control urination and can improve UUI symptoms.
- Bladder training: This technique involves gradually increasing the time between urination, helping the bladder to hold more urine, and reducing the urgency to urinate.
- Medications: Several medications can help manage UUI, including anticholinergics, beta-3 adrenergic agonists, and tricyclic antidepressants. These medications work by relaxing the bladder muscles, increasing bladder capacity, and reducing the frequency of involuntary contractions.
- Percutaneous tibial nerve stimulation (PTNS): This minimally invasive procedure involves the stimulation of the tibial nerve, which runs down the leg and controls bladder function. Electrical impulses are sent through a small needle inserted near the ankle, helping to regulate bladder activity and reduce UUI symptoms.
- Sacral neuromodulation (SNM): This treatment involves implanting a small device under the skin that sends electrical impulses to the sacral nerves, which control bladder function. This can help reduce UUI symptoms by modulating nerve signals between the bladder and the brain.
- OnabotulinumtoxinA (Botox) injections: Botox injections can treat severe UUI that doesn’t respond to other treatments. The injections relax the bladder muscles, reducing involuntary contractions and increasing bladder capacity.
- Surgery: In cases where conservative treatments are ineffective, surgery may be considered. Surgical options include sling procedures, bladder augmentation, and artificial urinary sphincter implantation.
Prevention of Urgency Urinary Incontinence
While it may not always be possible to prevent urgency urinary incontinence, certain measures can help reduce the risk or severity of symptoms. These include:
- Practicing pelvic floor exercises: Regularly performing Kegel exercises can help strengthen the pelvic floor muscles and improve bladder control.
- Maintaining a healthy weight: Obesity can contribute to UUI, so maintaining a healthy weight through a balanced diet and regular exercise can help prevent or alleviate symptoms.
- Avoiding bladder irritants: Limiting the intake of caffeine, alcohol, and acidic or spicy foods can help reduce bladder irritation and UUI symptoms.
- Managing chronic conditions: Proper management of conditions such as diabetes, neurological disorders, and hormonal imbalances can help prevent or reduce the risk of developing UUI.
Find The Right Treatment Option For You
Although urgency urinary incontinence can significantly impact your quality of life, it doesn’t have to be something you must manage for the rest of your life. From lifestyle modifications and pelvic floor exercises to medications, minimally invasive procedures, and surgical interventions, there is a range of approaches available to treat and prevent urgency urinary incontinence.