What Is Peyronie’s Disease?
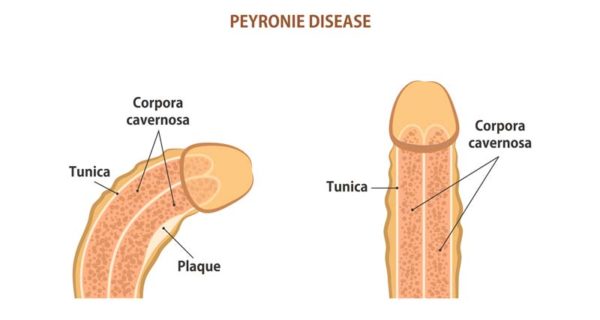
Peyronie’s disease is an abnormal curvature of the penis. It’s a relatively common condition that happens when plaque or scar tissue builds up in the penis and creates a curve in the penis during an erection. The plaque can also lead to painful erections or cause difficulty with sexual intercourse.
Causes of Peyronie’s Disease
The exact cause of Peyronie’s disease remains unknown, but several factors are believed to contribute to its development. It is thought that trauma or injury to the penis, such as during sexual activity or an accident, can trigger scar tissue formation. Other potential causes include genetic predisposition, autoimmune disorders, and abnormal healing processes within the penile tissue.
Symptoms
The most common symptom is penile curvature or bending, which can range from mild to severe. The curvature may be upward, downward, or to either side. In addition to the curvature, individuals with Peyronie’s disease may experience pain or discomfort during erections, which can lead to anxiety and difficulty with sexual activity. Some individuals may be able to feel scar tissue beneath the skin of the penis.
Diagnosis
Diagnosing Peyronie’s disease typically involves a comprehensive evaluation of the patient’s medical history, a physical examination, and additional tests. During the physical exam, a healthcare provider will assess the curvature of the penis, palpate the plaque or scar tissue, and inquire about any pain or discomfort experienced during erections.
In some cases, additional tests may be necessary to confirm the diagnosis or assess the severity of the condition. These tests may include ultrasound imaging of the penis to locate the plaque and determine its size. Blood tests may be necessary to rule out other underlying conditions.
Peyronie’s Disease Treatment
The management of Peyronie’s disease depends on the severity of symptoms and their impact on a person’s quality of life. While there is no cure for Peyronie’s disease, several treatment options are available to alleviate symptoms and improve sexual function. The choice of treatment will be tailored to each individual’s specific case, considering factors such as the extent of penile curvature, the presence of pain, and overall health status. Some men wonder if there is treatment for Peyronie’s disease without surgery. There are several effective treatment options before surgery, depending on the severity.
Here are some of the treatment options available:
1. Medications
- Collagenase Clostridium Histolyticum (CCH) Injections (Xiaflex): CCH is an enzyme that can help break down the fibrous scar tissue responsible for penile curvature in Peyronie’s disease. This injectable medication is administered directly into the plaque, softening the tissue and reducing the curvature. The treatment typically involves a series of injections over several weeks.
- Oral Medications: Some oral medications, such as vitamin E, potassium para-aminobenzoate (Potaba), and certain calcium channel blockers, have been used. However, their effectiveness remains a subject of debate, and they may not be as potent as other treatment options.
2. Physical Therapy
- Penile Traction Devices: Penile traction therapy involves using mechanical devices that gently stretch the penis over time. These devices can be worn discreetly under clothing and are designed to reduce penile curvature. The treatment duration may range from a few months to a year, depending on the severity of the curvature.
- Vacuum Erection Devices (VED): VEDs are cylindrical devices that create a vacuum around the penis, drawing blood into the erectile tissues to achieve an erection. Some studies suggest that regular use of VEDs may help preserve penile length and improve curvature in Peyronie’s disease.
3. Surgery
Surgical intervention is considered when conservative measures fail or in severe cases of Peyronie’s disease. Several surgical options are available, and the choice of procedure depends on the extent of curvature and other penile abnormalities. Surgical procedures may include:
- Penile Plication: This procedure involves making small incisions on the side of the penis opposite the plaque. Sutures are then used to “plicate” or gather the tissue, reducing the curvature.
- Excision and Grafting: In cases of severe curvature or large plaques, surgical excision of the plaque may be performed. To maintain penile length and rigidity, a graft (often from another part of the body or synthetic material) is used to replace the tissue that was removed.
- Penile Implants: In cases where Peyronie’s disease coexists with severe erectile dysfunction, penile implants may be considered. These implants are surgically inserted into the penis to provide a rigid erection.
4. Shockwave Therapy
Extracorporeal Shockwave Therapy (ESWT) involves using high-frequency shockwaves to break down the plaque and promote tissue healing. While research is ongoing, some studies suggest that ESWT may help improve penile curvature and alleviate pain associated with Peyronie’s disease.
5. Counseling
Dealing with this disease can be emotionally challenging, and counseling or therapy may be beneficial. A mental health professional can offer support and guidance to help individuals cope with the emotional impact of the condition, address any body image issues, and improve overall well-being.

