If your current Overactive Bladder (OAB) treatment isn’t working or you can’t tolerate it, ask your doctor if BOTOX® can help reduce unwanted leakage interruptions
BOTOX® Treatment For The Bladder
Botox (Botulinum A toxin) is a powerful drug that acts to temporarily paralyze muscles when it is locally injected. Botox is known for its popular use in cosmetics, but it actually has far-reaching medical applications. It is commonly used for diverse conditions like muscle spasticity, headaches, as well as the treatment of urinary incontinence.
Botox is a well-tolerated treatment and the application of this therapy ranges from simple conditions like overactive bladder to treatment of severely spastic bladders from neurologic disease. In many instances, Botox can be injected in a short procedure in our clinic. The therapy lasts for six to eight months and then is re-injected. There is no limitation to the duration of using this type of therapy.
You may have already tried OAB medication
Did you discover that your OAB medications:

BOTOX® is different from other treatments
BOTOX® is placed in the bladder muscle about every 6 months to target the source of your OAB
- In your body, certain chemicals travel from nerve cells to muscle cells to make your bladder contract so that you can urinate
- For people who have OAB, these muscles contract uncontrollably, creating leakage,the strong sudden need to go, and going too often
- BOTOX®is placed directly in the bladde rmuscle, where it helps block the nerve signals that trigger OAB
Proven to work when other OAB medications did not
In 3 clinical trials, 3 months after treatment, compared to placebo, BOTOX® significantly reduced daily leakage episodes
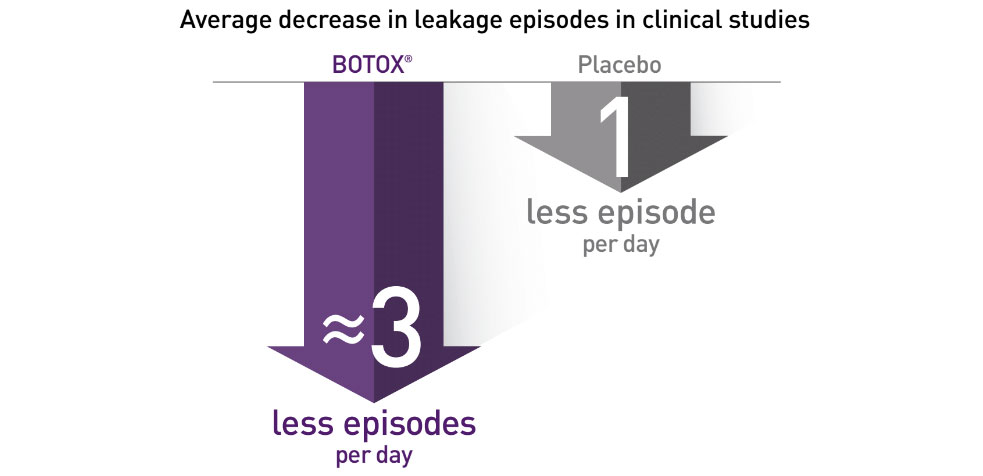
BOTOX® reduced leakage episodes by half or more
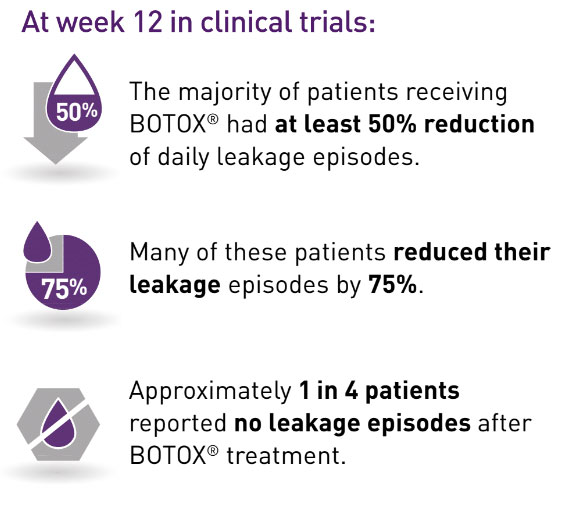
Patients in BOTOX® clinical trials reported improvement in their overall quality of life based on 3 categories:

Such as over planning every detail of your day in advance, worrying about where bathrooms are, and limiting how much fluid you drink.

Such as being preoccupied or frustrated with how your condition impacts your everyday decisions, such as what you can wear, where you can go, and how you feel about your overall well-being.

Such as being embarrassed or worried that your symptoms might be noticed by others.
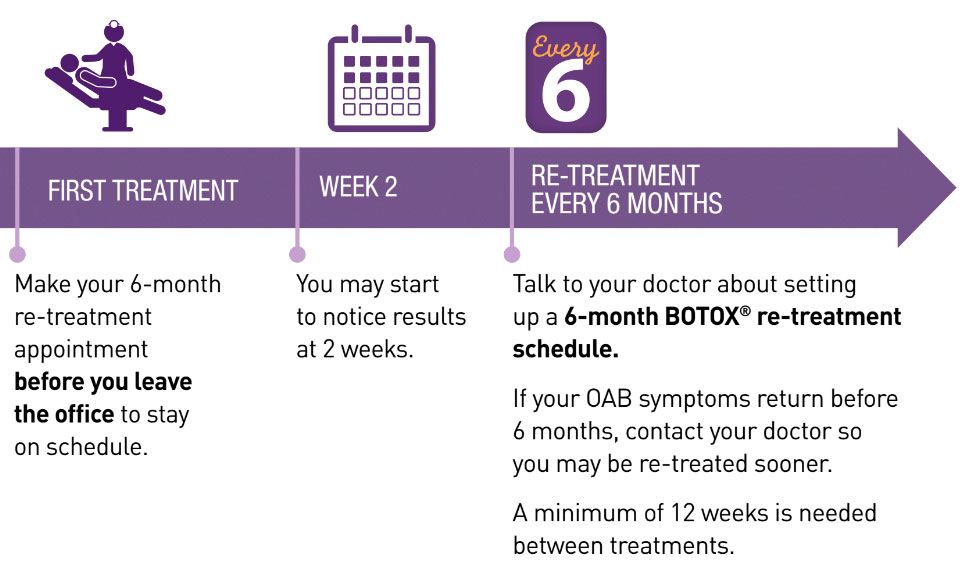
BOTOX® may be given in the comfort and convenience of your doctor’s office
The entire process takes about 1 hour
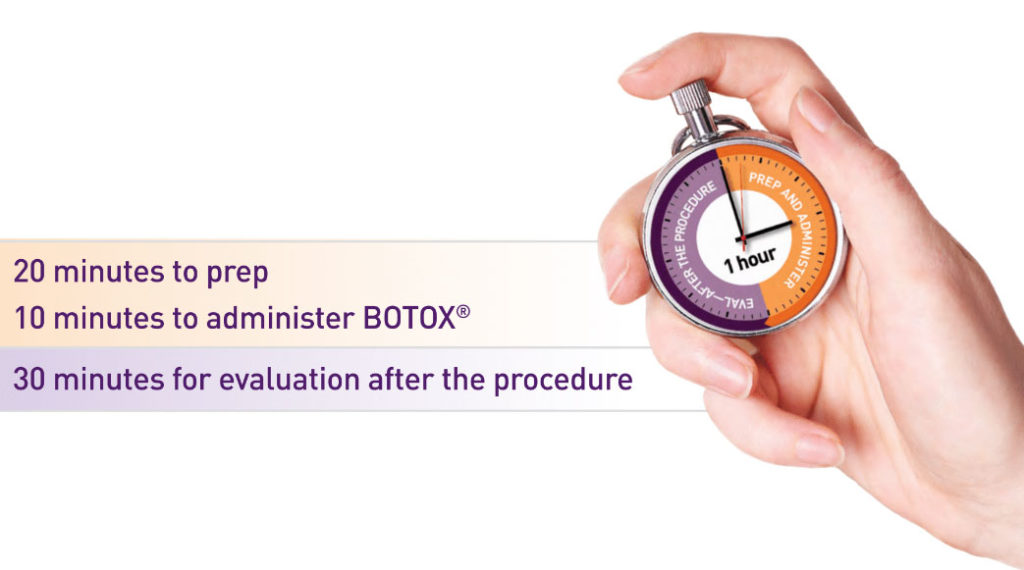
Plan on BOTOX® re-treatment about every 6 months
OAB is chronic and requires ongoing treatment